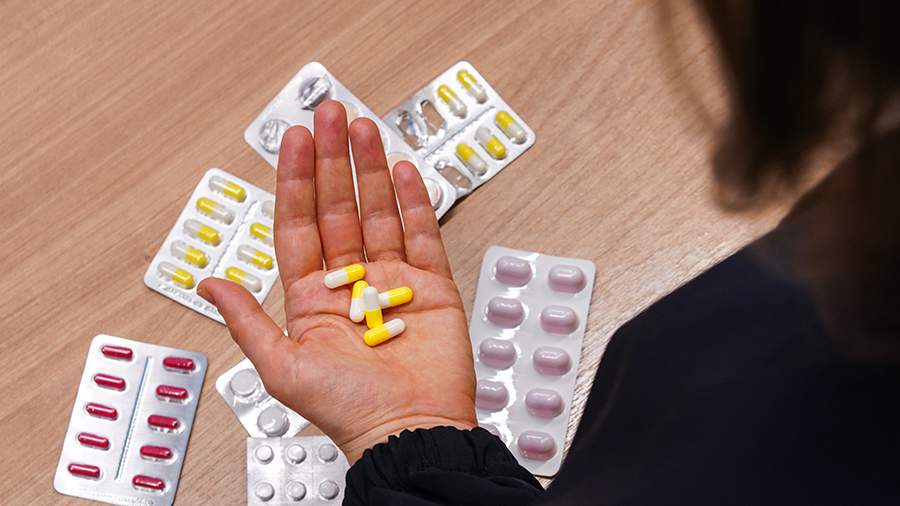
The All-Russian Union of Patients has voiced concerns that a new “second superfluous” rule in state procurement of medicines could impact around 200 crucial drug names. This regulation, favoring Russian pharmaceutical manufacturers, potentially limits access to essential treatments.
The All-Russian Union of Patients is raising an alarm regarding the “second superfluous” rule, set to take effect on September 1st, concerning public drug procurement. This rule grants preference solely to Russian pharmaceutical manufacturers operating a full production cycle.
The Union believes this rule will impact medications on the list of strategically important drugs, including essential and vital ones. This restriction could affect 215 positions, among which are drugs for oncological diseases. Yan Vlasov, Co-Chairman of the All-Russian Union of Patients, explained the potential risks:
Yan Vlasov, Co-Chairman of the All-Russian Union of Patients:
The “second superfluous” rule poses a significant threat to drug accessibility. While approximately 75-80% of medicines currently consumed in Russia are domestically produced copies or generics, the remaining vital drugs are largely sourced from abroad as originals. Even when certain drugs are deemed interchangeable, individual patient needs vary, and a generic does not always provide the same efficacy as the original. We advocate for the availability of all necessary medications, empowering doctors to select the most appropriate treatment. This rule risks limiting procurements to only domestic drugs, even when a patient requires a specific medication that may not be produced in Russia. Furthermore, there`s a concern that some manufacturers might neglect quality without sufficient investment, leading to additional problems for patients.
According to media reports, the Union has sent a letter to the government requesting a review of the drug categories affected by the “second superfluous” rule. The Cabinet of Ministers informed the publication that the appeal was forwarded to the Ministry of Industry and Trade and the Ministry of Health. The letter`s content is not publicly available, and some experts note that the information presented in the media currently appears somewhat ambiguous.
Dmitry Kulish, Professor at Skoltech and Director of the “Technological Entrepreneurship and Corporate Innovations” program, stated that while there are ongoing discussions about pharmacovigilance, intellectual property, and pricing mechanisms, these are not directly related to the “second superfluous” rule:
Dmitry Kulish, Professor at Skoltech, Director of “Technological Entrepreneurship and Corporate Innovations” program:
Most industry professionals define an `original drug` as a patented medicine with an active patent. If a domestic drug procured by the state infringes on such a patent, that`s a separate legal issue unrelated to the `second superfluous` rule. Many commercial entities also label drugs as `original` even after their patent protection has expired and generic equivalents exist. These so-called `original` drugs benefit from extensive pharmacovigilance data, which reassures doctors and officials about their efficacy. This then leads to discussions about pricing and the economic importance of generics. The global consensus is that generics are the backbone of the pharmaceutical industry; without them, monopolies emerge, leading to higher costs and reduced access for patients. Therefore, the critical question for regulators is the required extent of pharmacovigilance data for a generic to compete with an originator, given the latter`s vast pharmacovigilance history – a complex issue distinct from the `second superfluous` rule. A third point, raised by journalists referencing the Patients` Union letter, is the claim that many medications for chronic conditions, particularly in oncology, rheumatology, and blood disorders, cannot be abruptly switched. To validate this claim, one would need medical evidence demonstrating patients who experienced health issues after being forced to switch drugs, with such incidents properly monitored by pharmacovigilance. If such evidence were provided, we would acknowledge that the drug indeed has no true analogue, and the `second superfluous` problem would disappear. If we definitively know a patient cannot be easily switched from drug A to drug B, even if they share the same name, mechanism, and indications, then they are, in fact, different drugs, and the `second superfluous` rule would again be inapplicable.
Currently, the list of vital medications comprises nearly 900 international non-proprietary names (INN), or 6,800 trade names, according to a report by “Cursor,” an IT company specializing in pharmaceutical tender procurement analysis. Of these, 70% are locally produced: 40% manufactured by Russian companies using imported substances, and 30% from Russian-sourced substances.